상고실 내벽 및 전벽에 발생한 다발성 추골 고정에 대한 병합 접근법
Combined Approach for the Multiple Fixations of the Malleus to the Medial and Anterior Epitympanic Wall
Article information
Trans Abstract
Malleus fixation leads to conductive hearing loss and is a major cause of persistent hearing loss after stapes surgery. It is difficult to visualize and manage malleus fixation to the medial epitympanic wall using an operating microscope. This report describes the case of a 50-yearold woman who was successfully treated with a combined surgical approach. The patient underwent a combined microscopic and endoscopic malleostapedotomy for the surgical correction of multiple malleus fixations to the medial and anterior epitympanic wall along with stapes fixation. The combined surgical technique enabled direct visualization and removal of the fixed lesion with limited atticotomy. The postoperative average air-bone gap was within 20 dB. The study thus showed that combined approach can help minimize the extent of atticotomy as well as identifying and removing the fixed lesion under direct magnification. It is a viable option for the surgical treatment of malleus fixation to the medial epitympanic wall.
Introduction
Malleus fixation can occur on its own or in combination with other ossicular fixations [1].When malleus fixation accompanies other ossicular fixations, the stapes is often involved. Concurrent malleus and stapes fixation can be difficult to diagnose preoperatively or intraoperatively, and it is the main cause of persistent conductive hearing loss after primary stapes surgery [2]. Malleostapedotomy is required for the treatment of mallear and stapedial fixation. It is usually performed via an endaural approach using an operating microscope [2]. However, it is difficult to observe a fixed lesion directly when the malleus is fixed to the medial epitympanic wall. In addition, removal of the fixed lesion between the malleus and the medial epitympanic wall cannot be achieved solely via microscopic view.
Endoscopic surgery has become popular in the field of otology with the advancement of optical and medical engineering technologies. Various otologic procedures, such as ossiculoplasty and intralabyrinthine schwannoma excision, have been performed using an endoscope alone or in conjunction with a microscope (combined approach) [3,4]. An endoscope allows close observation of the ossicles and various hidden areas in the middle ear, thereby providing a wide and magnified view. Considering these advantages, an endoscope would be helpful in the management of malleus fixation to the medial epitympanic wall.
Herein, we describe a case of malleus fixation at multiple sites (medial and anterior epitympanic walls) along with stapes fixation, which was performed using a combined microscopic and endoscopic approach.
Case
A 50-year-old woman presented with hearing loss on the right side since childhood. Physical examination revealed an intact tympanic membrane. Pure-tone audiometry of the right ear showed an air-bone gap of 45 dB on average from 0.5 to 3 kHz (Fig. 1A). Axial temporal bone computed tomography scan showed bony bridges between the malleus head and medial and anterior epitympanum (Fig. 1B and C). No otospongiotic foci were detected in the scans. Under general anesthesia, an endaural approach was used under microscopic view. A tympanomeatal flap was elevated, and the middle ear was exposed. Ossicular mobility was checked, and the malleus was fixed. After separating the incudostapedial joint, the mobility of the incus and stapes was rechecked. The stapes was also fixed. A limited atticotomy was performed with a curette and burr for better visualization of the epitympanum. The endoscope was then introduced, and the ossicular status in the epitympanum was examined using a 0 or 30 degree endoscope. A bony bridge was observed between the malleus head and the medial epitympanic wall, which made the malleus immobile. The endoscope was used to completely visualize this. The malleus was also fixed to the anterior epitympanic wall due to a similar bony bridge being present between the two structures (Fig. 2A and B). The fixed malleus head was freed from the surrounding epitympanic wall by fracturing the bony bridges using microinstruments (Fig. 2C and D) and removed using a malleus nipper (Fig. 2E and F). The tympanic membrane attachment to the malleus handle was separated approximately 1 mm caudal to the lateral process of the malleus. The incus was removed, and the stapes suprastructure was cut using crurotomy scissors. Under microscopic view, adequate length of the piston and inclination were estimated using a measuring rod and the 0.4 mm Fisch titanium stapes piston. The stapes footplate was fenestrated, and the piston was inserted into the stapes footplate opening. The piston loop was crimped to the malleus handle. The insertion site was sealed using harvested pieces of soft tissue and glue. Attic reconstruction was performed using harvested tragus perichondrium and cartilage. The tympanomeatal flap was restored to its original location. The postoperative course was uneventful, and the pure-tone audiogram at 6 months showed 12.5 dB of air-bone gap on average from 0.5 to 3 kHz, with a 32.5 dB closure of the preoperative air-bone gap (Fig. 3).
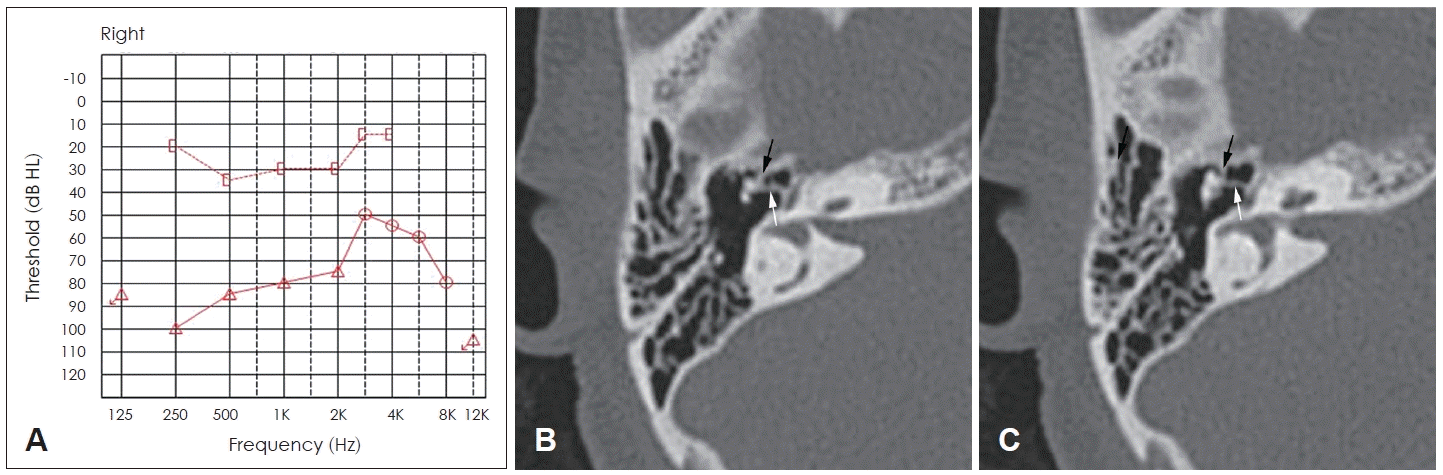
Preoperative pure-tone audiogram and temporal bone computed tomography imaging. The average air-bone gap at 0.5 kHz, 1 kHz, 2 kHz, and 3 kHz is 45 dB, indicating conductive hearing loss (A). Axial scan shows bony bridges between the malleus head and anterior (black arrow) and medial (white arrow) epitympanic walls (B and C).

Intraoperative endoscopic finding. The bony bridges between the malleus head and the anterior epitympanic wall (Ae) (arrow) and medial epitympanic wall (arrowheads) make the malleus immobile (A). Endoscope enables the medial bony bridge to be visualized completely (B). The bony bridges are fractured using microinstruments (C and D). The malleus head is amputated (E) and removed (F). Mn, malleus neck; Tt, tegmen tympani.
Discussion
Fixation between the malleus and epitympanum often occurs at the anterior, superior, or lateral wall of the epitympanum [5]. This fixation is usually caused by hyalinization or calcification changes of the corresponding mallear ligaments (anterior, superior, or lateral) [5-7]. In the present study, the malleus head was fixed to the anterior and medial epitympanic walls (Fig. 1B and C). Although congenital malleus fixation at multiple sites of the epitympanic wall has been described in previous reports, to our knowledge this is the first case successfully managed using a combined microscopic–endoscopic approach.
Malleus fixation is often secondary to trauma, chronic otitis media, and tympanosclerosis, with tympanosclerosis being the most common cause [8]. However, it can occur congenitally and idiopathically, as in the present case. In a previous study including 168 patients with malleus fixation who underwent middle ear surgery over 5 years, idiopathy was the second most common cause following tympanosclerosis, which accounted for 39.2% of the cases. Among them, 8.9% of patients had accompanying otosclerotic stapes fixation [8]. This idiopathic malleus fixation was also revealed in a temporal bone histopathologic study. Bony fixation of the malleus was observed in 14 (1.3%) out of 1,108 temporal bones, and the aforementioned secondary causes did not exist in all cases [5].
Two surgical methods have been used to treat malleus fixation. One method is to remove the malleus head and the incus, followed by reconstruction of the ossicular chain using either the incus that was removed or ossicular prosthesis. The second method involves ossicular mobilization. The fixed lesion is drilled away, and a gap of approximately 2 mm is created between the malleus and the epitympanum while maintaining the continuity of the natural ossicular chain. This method is more physiological than the first method, as the natural mechanism of sound conduction is preserved. However, a recent meta-analysis demonstrated no significant differences in postoperative hearing outcomes between the two methods [9]. The second method is difficult to use when the malleus is fixed to the medial wall of the epitympanum. In the present case, we removed the malleus head to minimize the risk of postoperative refixation because the fixation involved multiple epitympanic walls, despite releasing the fixed lesions completely.
The postoperative hearing outcomes of malleostapedotomy are favorable, regardless of the disease etiology. A previous study on revision stapes surgery for otosclerosis reported that 77% of patients who underwent malleostapedotomy had an air-bone gap of less than 20 dB after surgery. Among them, 46.2% of the patients had accompanying malleus fixation, and their postoperative hearing results were not different from that of those in whom malleostapedotomy was performed for other causes. Moreover, the outcome at a low frequency was superior to that of standard incudostapedotomy [2]. In another study, more than 80% of the participants had an air-bone gap within 20 dB for revision malleostapedotomy and primary malleostapedotomy [6]. The postoperative outcomes in the present case were similar to those reported in the previous studies. The bone conduction thresholds in pure-tone audiometry did not increase after the surgery, and the air-bone gap was 12.5 dB with a 32.5 dB closure of the preoperative air-bone gap.
In conclusion, malleostapedotomy can be performed successfully using a combined microscopic and endoscopic approach in patients with malleus fixation to the epitympanic walls, along with stapes fixation. The combined approach can help minimize the extent of atticotomy, as well as identify and remove the fixed lesion under a direct magnified view. In particular, it is a viable option for surgical treatment of malleus fixation involving the medial epitympanic wall.
Notes
Acknowledgments
None
Author Contribution
Conceptualization: Jin Woong Choi. Data curation: Jin Woong Choi. Formal analysis: Sumin Yi. Investigation: Jin Woong Choi. Methodology: Sumin Yi. Project administration: Jin Woong Choi. Resources: Jin Woong Choi. Software: Jin Woong Choi. Supervision: Jin Woong Choi. Validation: Jin Woong Choi. Visualization: Sumin Yi. Writing—original draft: Sumin Yi. Writing—review & editing: Sumin Yi, Jin Woong Choi.

